Here's How America Let 70,000 Opioid-Related Deaths Go Unaccounted For
One four-digit code is potentially hiding thousands of opioid-overdose deaths.
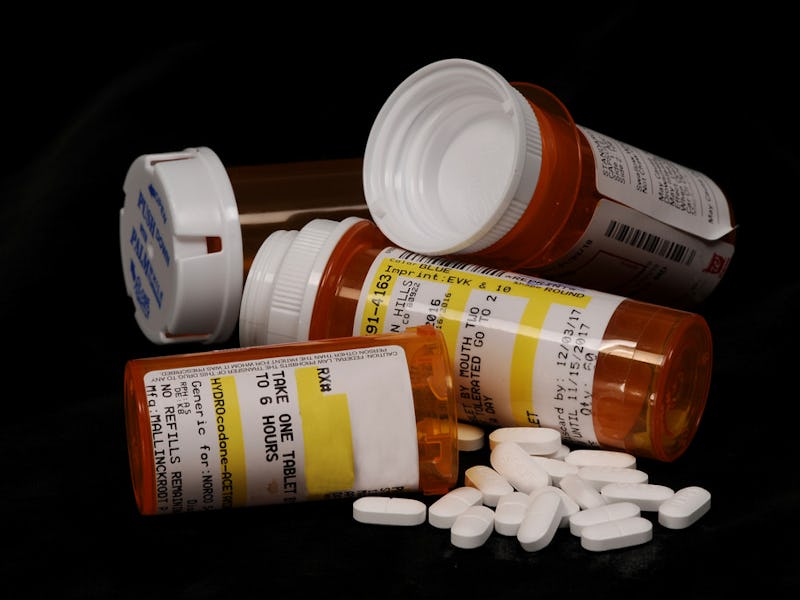
The rate of overdose deaths due to opioids is already alarmingly high, killing 40,000 people in the United States in 2016 alone. But a study published Wednesday in Public Health Reports suggests even that number might be a gross underestimate. The University of Pittsburgh biostatisticians behind the study combed through death certificates from all fifty states, looking for places where opioid deaths might have been miscounted. What they found was nearly 70,000 potentially mislabeled deaths from 1999 to 2015, lurking in the fine print.
When we underestimate the number of people who died from opioids, we are more likely to underestimate the severity of the problem. This is evident in the paper, which cites data accumulated by the National Center for Health Statistics from 1999 through 2015 showing that nearly 500,000 people died of drug overdoses in general, from drugs ranging from opioids to psychotropics. From there, the team broke the causes of death down into three different buckets: opioid-related overdoses, non-opioid related overdoses, and a nebulous category called “unspecified.” Of those 500,000 overdose deaths, 58 percent of those were attributed to opioids, but 22 percent of them were classified as “unspecified.” A closer look at those “unspecified” cases suggested it contained 70,000 people who died from opioid overdose but were never counted as opioid-related deaths. In five states in particular, Alabama, Indiana, Louisiana, Mississippi and Pennsylvania, the team estimates that up to 35 percent of all opioid-related deaths were lurking in this “unspecified” limbo.
A closer look at those death certificates revealed noticed a pattern — a recurring four-digit code, “T50.9,” that lead study author Jeanine Buchanich, Ph.D. tells Inverse may hold the key to tracking these deaths in the future.
The black bars represent the amount of overdose deaths labeled "unspecified" in 2015. The dark gray bars shown overdose deaths attributed to opioids and the light gray bars show overdose deaths due to other non-opioid drugs.
To understand how this underreporting happens, you have to know a little bit about what happens to someone after they’re declared dead due to a drug overdose. Buchanich isn’t a toxicologist or medical examiner, but she is a biostatistician, and her research illuminated a few holes in the post-mortem chain of command. “Often medical examiners and coroners must await toxicology results and then go back to the death certificate and add the drug information,” she says.
The point of a toxicology report is to help identify what drug causes the overdose. It comes down to the issue of what the authors call “drug specificity,” which can be useful in compiling statistics on which drugs are associated with overdose deaths. Once a toxicology report is compiled, it is sent back to the medical examiner or coroner where it’s up to them to interpret the results.
“Coroners or medical examiners can complete death certificates,” Buchanich says, “but coroners are less likely to be physicians and do not necessarily have the medical training useful for completing drug information on death certificates based on toxicology reports.”
Buchanich is referring to the fact that you don’t actually have to be an MD to get a job interpreting cause of death. In places like Indiana, coroners are simply elected and don’t necessarily need to have any training in forensic pathology. Medical examiners, on the other hand are often degree-wielding doctors, some of whom have expertise in forensic pathology. But according to Kim Collins, president of the National Association of Medical Examiners (NAME), there aren’t many of these experts to go around.
“There are several challenges,” Collins says, “such as a marked shortage of forensic pathologists to perform medicolegal death investigations and certify cause and manner of death,” she tells Inverse via email. This is echoed in a report by the Society of Medicolegal Death Investigations from 2012 showing that only 30 to 40 out of 17,000 medical school graduates would become forensic pathologists.
This gap expertise is important because the coroner, medical examiner, or hopefully, forensic pathologist, is responsible for a crucial step when it comes to reporting an overdose on a death certificate: assigning the International Classification of Diseases code that represents cause of death. Drug-specific overdoses are written as a “contributing cause” on the death certificate and noted by a class of codes called “T-codes.” Many drugs have their own specific T-code, which helps the NIH track which drugs are leading the charge when it comes to overdose deaths. For instance, if someone dies of an opium overdose, their death would be coded as a T40.0.
But if there’s also a catch-all T-code called T50.9, which is used when the overdose death is caused by “other and unspecified drugs, medicaments and biological substances.”
There should be a cause of death and a specific T-code listed in the "cause of death section' on death certificates in the case of a drug overdose.
It’s up to a coroner or medical examiner to assign this T-code. Some use T50.9 in combination with other codes to help describe drugs that don’t have a code assigned by the NIH, like bath salts, but this research suggests that a death certificate with T50.9 alone is a bit of a red flag. It means that the person died of a drug overdose but that, for whatever reason, the coroner never officially identified the drug. The University of Pittsburgh team says that if you apply the proportion of opioid-related overdose deaths (58 percent) to the number of these certificates labeled with the code T50.9, you could estimate the number of these “unspecified” deaths that were actually caused by opioids. That’s where they found their estimated 70,000 additional deaths.
Why might this T509 code be so ubiquitous? According to this paper, states that rely on a county coroner system were more likely to use this T50.9 code, leaving the drug responsible for death a mystery when it might well have been an opioid. “States with a decentralized county coroner system, such as Louisiana, or with a hybrid system that involved county coroners and state medical examiners, such as Pennsylvania, were likely to have a higher proportion of overdose deaths with unspecified drug codes,” Buchanich says.
Indiana, for example, stands out: When Buchanich and her team team factored the deaths to to “unspecified” drug overdoses into the overall opioid mortality rate Indiana had the 15th highest opioid-overdose mortality rate in the country. Before the analysis, it was 34th.
A map showing the breakdown of states with coroner systems, medical examiner systems, and "hybrid systems.'
The NAME suggests that each and every drug overdose death should be reviewed by people with the appropriate expertise. They have exacting standards intended help medical examiners follow the guidelines needed to correctly assign T-codes and perform full post-mortem investigations. But as the researchers demonstrated, this doesn’t always happen, particularly in states that don’t have a medical examiner system solidly in place.
That said, Buchanich and her team make it clear that it’s actually getting harder and harder to assign T-codes to drug overdose deaths – even for experts. For instance, Collins notes that certain “designer drugs” that are chemically more complicated might make it harder for medical examiners or coroners identify certain opioids in toxicology results. This, Buchanich adds, might lead to continued underreporting of opioid deaths from synthetic opioids, like fentanyl
But for now, we have a decentralized system, a catch-all code, and potentially 70,000 more tragic overdose deaths to grapple with.