MRI Scans Reveal Differences in Brains of People With Anxiety and Depression
These debilitating conditions have a physical basis.
In the United States, approximately 16 million adults are diagnosed with major depression disorder and about 15 million adults have social anxiety disorder. While the disorders are different — people with depression often feel persistent sadness and lose interest in things they once cared about, and those with anxiety have an intense fear of being watched and judged — some of the most debilitating clinical symptoms of depression and anxiety overlap.
New research, which will be presented next week at the annual meeting of the Radiological Society of North America, is the first evidence that this overlap may be caused by similar structural abnormalities people with depression and social anxiety have in their brains. While the paper is not published yet, the abstract is available online.
A team of doctors from Sichuan University in Chendgu, China discovered that patients with depression and anxiety both have abnormalities in the grey matter of their brains’ salience and dorsal attention networks. The salience network determines what stimuli catch the attention of the brain, and the dorsal attention network drives focus and attention.
“These consistent structural differences in the two patient groups may contribute to the broad spectrum of emotional, cognitive, and behavioral disturbances observed in MD [major depression] and SAD [social anxiety disorder] patients,” the doctors write. “These findings provide new evidence of shared and specific neuropathological mechanisms underlying MDD [major depressive disorder] and SAD.”
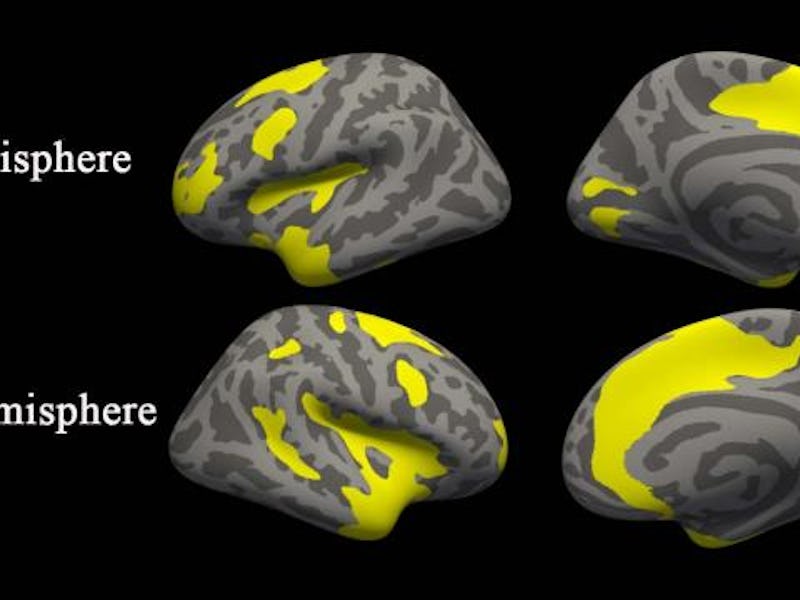
MRI scans showed differences in cortical thickness between people with MDD or SAD and healthy controls (HC).
In the study, which uncovered the first preliminary evidence of the gray matter changes in the brains of MDD and SAD patients, the researchers used magnetic resonance imaging (MRI) to evaluate the brains of 37 MDD patients, 24 SAD patients, and 41 healthy control individuals.
Compared to the control participants, MDD and SAD patients showed a cortical thickening in the brain’s insular cortex, which influences perceptions of empathy, self-awareness, and interpersonal experiences. This thickening, study co-author Youjin Zhao, M.D., Ph.D., explains in a statement, may be a result of inflammation and could “be the result of both the continuous coping efforts and emotion regulation attempts of MDD and SAD patients.”
The researchers found differences between the brains of people with MDD and SAD, too. Brains of patients with depression showed alterations in the regions of the brain that control emotional facial processing, while brains of patients with anxiety had “disorder-specific involvement” in the regions associated with processing fear.
What the exact relationship between these disorders and the cortical thickening of the brain, particularly in the anterior cingulate cortex, remains to be understood. More studies with larger sample sizes that use machine learning analysis, are needed, says Zhao — but there may be a future where MRIs can help aid the diagnosis of these widespread, debilitating conditions.
If you liked this article, check out this video of LSD’s effects on the brain.