How New HPV Findings Change What Many Thought About the Vaccine
There are hopeful signs that the cancer-causing virus will one day be eliminated.
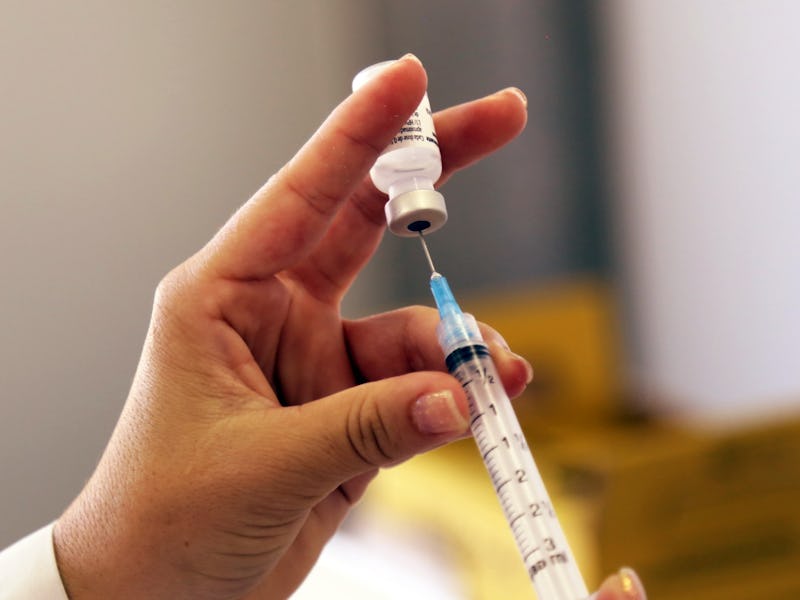
More than 10 years have passed since the human papillomavirus (HPV) vaccine became publicly available. During that run, its safety, legitimacy, and side effects have been questioned by concerned parents and the media. However, a study released Wednesday in The Lancet firmly establishes that the vaccine really works — so much so that it could lead to the eradication of cervical cancer.
“The impact of the HPV vaccination has actually exceeded expectations,” says co-author Lauri Markowitz, MD, associate director of science for HPV at the Centers for Disease Control and Prevention. “The trials showed that HPV vaccines are very effective, and data from the real world has confirmed that.”
On Track to Cervical Cancer Elimination
The Lancet paper is a review of 65 studies that includes more than 60 million people living in 14 countries, each of which has set up HPV vaccine programs in the last decade. These studies allowed Markowitz and colleagues to compare the frequency of HPV infections, anogenital warts, and precancerous cervical lesions before and after the programs were launched.
The studies themselves spanned an eight-year period and revealed that, in that time, overall infections have dropped by 83 percent among girls between the ages of 13 and 19, and 66 percent among women between the ages of 20 to 24. Meanwhile, anogenital warts dropped by 67 percent among 15- to 19-year-old girls; by 54 percent among women aged 20 to 24; and by 31 percent for women aged 25 to 29. Furthermore, precancerous cervical lesions dropped by 51 percent among teenagers and 31 percent among young women.
A girl receives an HPV vaccine in Sao Paulo, Brazil.
Importantly, the researchers also saw positive signs of herd immunity. In countries where at least half of the population electable for the vaccination actually got the vaccination, there was a decrease in the prevalence of HPV-related diseases among those who were not vaccinated. For example, anogenital warts among males dropped by 48 percent for those aged 15 to 19 and by 32 percent for those aged 20 to 24.
“HPV vaccination is still too recent to directly measure its effect on cervical cancer, as it takes decades to develop,” explains co-author Mélanie Drolet, Ph.D., a senior research associate at Laval University. “However our analyses show that vaccination is production substantial reductions in the infections that cause cervical cancer and precancerous lesions.
“These reductions are a first sign that vaccination could eventually lead to the elimination of cervical cancer as a public health problem.”
Why This Is Important
While HPV infections and cervical pre-cancers (the abnormal cells on the cervix that lead to cancer) have dropped dramatically since the vaccine was introduced, they are still a major public health concern.
About 14 million people become infected with HPV each year. The virus has many strains, and, in turn, the strains cause different infections. While most of these infections go away on their own, the ones that don’t can cause certain types of cancer. As of now, HPV causes over 337,000 cases of cancer in men and women every year in the US. These include penile cancer, cervical cancer, and vaginal and vulvar cancers.
An illustration of the HPV virus.
Although many studies like the Lancet review have demonstrated the beneficial effects of the vaccine, uptake of the HPV vaccine remains slow. Currently, just 60 percent of American adolescents have received at least one dose of the HPV vaccine; typically, between two to three doses are required for full coverage.
Because of this, the CDC and other health researchers continue to encourage parents to vaccinate their sons and daughters. On Wednesday, a public health advisory panel advised people through the age of 45 to get an HPV vaccine, as they could still benefit from it. Currently, the most commonly used vaccine, Gardasil 9, protects against nine strains of HPV, seven of which are linked to 90 percent of HPV-related cancers.
While being vaccinated as a preteen is the ideal route, this panel notes that, for many adults, it’s not too late to protect oneself from these strains, even if you’ve had HPV before.
Partial abstract:
Method: In this updated systematic review and meta-analysis, we used the same search strategy as in our previous paper. We searched MEDLINE and Embase for studies published between Feb 1, 2014, and Oct 11, 2018. Studies were eligible if they compared the frequency (prevalence or incidence) of at least one HPV-related endpoint (genital HPV infections, anogenital wart diagnoses, or histologically confirmed CIN2+) between pre-vaccination and post-vaccination periods among the general population and if they used the same population sources and recruitment methods before and after vaccination. Our primary assessment was the relative risk (RR) comparing the frequency (prevalence or incidence) of HPV-related endpoints between the pre-vaccination and post-vaccination periods. We stratified all analyses by sex, age, and years since introduction of HPV vaccination. We used random-effects models to estimate pooled relative risks.
Findings: We identified 1702 potentially eligible articles for this systematic review and meta-analysis, and included 65 articles in 14 high-income countries: 23 for HPV infection, 29 for anogenital warts, and 13 for CIN2+. After 5–8 years of vaccination, the prevalence of HPV 16 and 18 decreased significantly by 83% (RR 0·17, 95% CI 0·11–0·25) among girls aged 13–19 years, and decreased significantly by 66% (RR 0·34, 95% CI 0·23–0·49) among women aged 20–24 years. The prevalence of HPV 31, 33, and 45 decreased significantly by 54% (RR 0·46, 95% CI 0·33–0·66) among girls aged 13–19 years. Anogenital wart diagnoses decreased significantly by 67% (RR 0·33, 95% CI 0·24–0·46) among girls aged 15–19 years, decreased significantly by 54% (RR 0·46, 95% CI 0.36–0.60) among women aged 20–24 years, and decreased significantly by 31% (RR 0·69, 95% CI 0·53–0·89) among women aged 25–29 years. Among boys aged 15–19 years anogenital wart diagnoses decreased significantly by 48% (RR 0·52, 95% CI 0·37–0·75) and among men aged 20–24 years they decreased significantly by 32% (RR 0·68, 95% CI 0·47–0·98). After 5–9 years of vaccination, CIN2+ decreased significantly by 51% (RR 0·49, 95% CI 0·42–0·58) among screened girls aged 15–19 years and decreased significantly by 31% (RR 0·69, 95% CI 0·57–0·84) among women aged 20–24 years.