Blood Plasma From Youth Successfully Invigorates Alzheimer's Patients
"I want to find a cure."
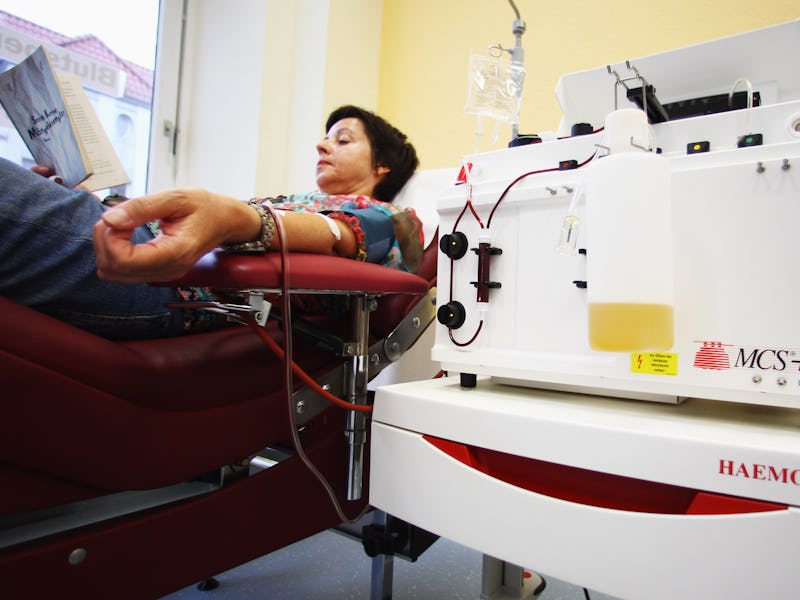
In 2014, a team led by Stanford neurologist Tony Wyss-Coray published a study that seemed more like science fiction than actual medicine. In Nature, they announced that they’d successfully transferred blood plasma from young mice into old mice in an attempt to improve their age-related cognitive problems — and the experiment was a success. Wyss-Coray went on to found a biotechnology company called Alkahest, which in 2016 took the research a step further by injecting blood plasma from young humans into older mice, a bold move that also resulted in improvements in mouse memory, cognition, and physical abilities.
These studies laid the groundwork for the research of Sharon Sha, M.D., a Stanford scientist who’s trying to use young blood plasma to treat people with Alzheimer’s disease, which severely impairs memory, thinking, and behavior in older people. On Saturday, Sha announced at the Clinical Trial on Alzheimer’s Disease conference that her team had successfully administered young plasma to people with the disease, who subsequently showed improvements in their ability to do basic tasks, like remembering to prepare meals and take medications.
Though the improvements were small, Sha’s latest findings provide strong support for Wyss-Coray’s original hypothesis. There’s something in young blood plasma that can restore youthful qualities to the old.
“Obviously, what we don’t want for people to take away from this study is that it’s time to ask their 18-year-old nephew to give them their blood so they can live forever,” Sha tells Inverse. “But the goal is really to say, number one, is this safe? And, number two, can we repeat this in a larger sample of patients?”
Two bags of frozen plasma, the liquid portion of the blood after blood cells, platelets, and other cellular components, are removed.
Sha’s PLASMA trial, which was designed to test Wyss-Coray’s original hypothesis, split up its 18 participants into two groups: The first received four weekly infusions of either plasma from young donors (between the ages of 18 and 30) or a placebo saline solution. After the weekly infusions and a six-week “washout period” in which no one received any infusions, the people who received plasma and those who received the placebo switched. The participants, who filled out questionnaires to test their mood, cognition, and functional ability throughout the infusion period, didn’t know which infusion they received at which time.
The second group of participants also received young-donor plasma infusions, but they knew they were getting them. They, too, filled out the questionnaires.
Sha’s analysis revealed that the transfusions weren’t just safe — they were also linked to statistically significant improvements in the smaller tasks that make daily living possible for these Alzheimer’s patients. Meanwhile, they didn’t seem to cause any significant changes in the participants’ moods or results on cognitive tests.
The trial is small, Sha admits, but what’s important is that the results warrant pursuing research in this admittedly strange field. Most big clinical trials last for at least a year and have thousands of patients. That’s not where Sha’s team is yet, but, bolstered by their recent successes, they soon very well could be.
Pushing forward, after all, is the only way to reveal the answer to what Sha calls the “million-dollar question”: What’s in young plasma anyway?
Dr. Sharon Sha
“Previous studies haven’t identified exactly what is in young plasma, but our guess is that there is some sort of milieu, so to speak, that is impacting maybe healing, regenerating — we’re not sure,” says Sha. “If we identify what’s in young plasma, we won’t have to necessarily rely on young donors. Until we do that, we might have to continue to use young donors to help us continue to study this.”
The hope, in other words, is that Sha’s team can determine what compounds are in plasma so that they can be recreated — perhaps artificially, or pulled from animal sources — and used to develop treatments for Alzheimer’s and other diseases. As of now, Sha says, her Alzheimer’s patients have no options for treatment.
“The majority of my time I see patients with Alzheimer’s disease and they ask me what I can do — everyone knows there’s no cure,” says Sha.
“My motivation is to be involved in clinical trials that think outside the box and find ways that we can actually improve the lives of people with Alzheimer’s disease and other disease.”
Peter Thiel is allegedly an early adopter of "young blood treatment" technology.
This extremely out-of-the-box approach to treating widespread diseases has, perhaps unsurprisingly, inspired a spirit of entrepreneurship among the scientists who are helping to develop it. Alkahest, which sponsored Sha’s study and owns the intellectual property behind the treatment regime, isn’t the only company to emerge from the young-blood mice studies. Another investigator involved in the original 2014 study, Jesse Karmazin, M.D., founded Ambrosia, a “young blood treatment” company that has attracted the attention of Silicon Valley tech elite like Peter Thiel.
But, as Sha and others in the field are diligent to point out, it’s important to keep in mind that this research is still in its extremely early stages, despite what some companies might try to sell to the public. Ambrosia, for one, has garnered the ire of Wyss-Coray, who told Science in 2016 that “there’s just no clinical evidence [that the treatment will be beneficial] and you’re basically abusing people’s trust and the public excitement around this.” While Sha’s work focuses on blood-based medical therapies for the sick, Ambrosia’s mission is to help the healthy stay that way, reinvigorating older people with the blood of the young in the hopes it will extend their lives.
Sha, for her part, doesn’t seem surprised that Silicon Valley types would be interested in this kind of research but emphasizes that her work is to aid people to become healthier, not live longer. Her goal is to try and help her patients — and there’s a chance that plasma infusions may one day help.
“With the research time I have,” says Sha, “I want to find a cure.”
If you liked this article, check out this video on how weed could cure Alzheimer’s.