This One Simple Trick Can Reduce Opioid Prescriptions
It's all about the power of suggestion.
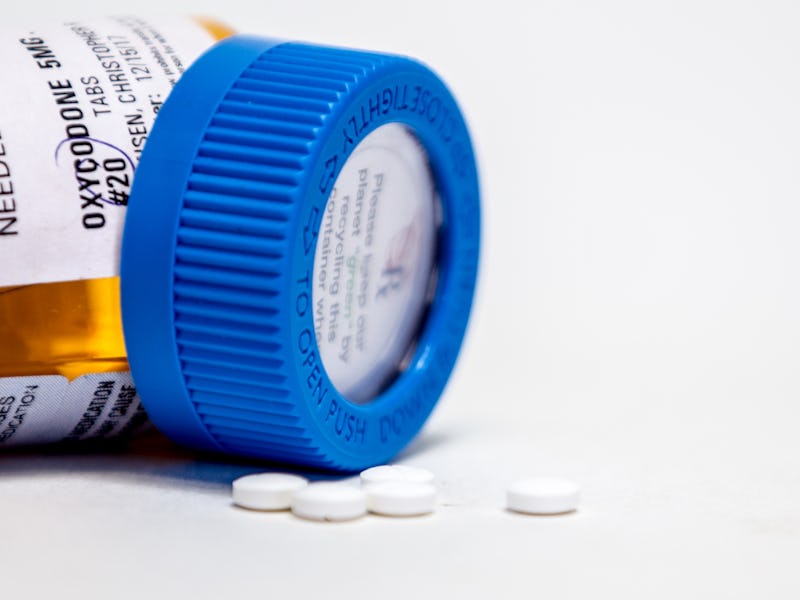
The United States is in the midst of an opioid crisis that continues to claim lives at an accelerating rate. Research suggests we may even be under-counting the number of opioid overdose deaths. And while the US Centers for Disease Control and Prevention says illicit synthetic opioids are driving the greatest increases in overdose deaths, doctors can’t ignore the role that medical prescribing practices play in fueling addiction. To address the medical community’s responsibility, new research in JAMA Surgery suggests a startlingly simple solution.
In a paper published Wednesday, a team of doctors led by first author Alexander Chiu, M.D., a surgical resident at Yale School of Medicine, shows that a small change in the way doctors prescribe opioids through electronic medical record software can be an effective way to get patients to take painkillers for less time. By lowering the “default” number of pills that the software suggests when doctors are writing prescriptions for patients from 30 to 12 after routine surgeries, they successfully lowered the average number of pills doctors prescribed.
In the three months before the change, the average number of opioid pills prescribed for postoperative patients was 30 across the five different hospitals involved in the study. But in the three months after the change, that number went down to 20. Before the change, 40 percent of prescriptions written at the study hospitals were for 30 pills, but after the change, only 13 percent were.
This result is promising, especially given a January 2018 paper published in the British Medical Journal, which shows that the length of time a patient takes opioids is a stronger predictor of addiction than the dosages prescribed. So even though changing the default levels of postoperative opioid prescriptions did successfully lower the total quantity of drugs by about 34 percent, more importantly, prescribing fewer pills means that patients are taking opioids for a shorter amount of time after their surgeries. And crucially, the change costs nothing to implement.
“Lowering the default number of opioid pills prescribed in an [electronic medical record] system is a simple, effective, essentially cost-free, and potentially wide-reaching intervention to change prescriber behaviors,” write the study’s authors. This kind of doctor-focused opioid intervention isn’t always a home run, though.
A major concern that’s come up in recent years is that, by focusing on prescribing practices as a way to fight the opioid crisis, doctors are making it harder for pain patients to get the relief they need. The new study’s authors say this did not appear to happen during their research, though.
Their results showed that patients got just as many refills after the software change as they had before, suggesting that a lower number of postoperative pills wasn’t making them suffer needlessly. Their next steps, they write, will be to find the sweet spot between pain management and overprescribing.
“Future study is warranted to identify an optimal default setting that minimizes opioid prescriptions while providing sufficient analgesia.”