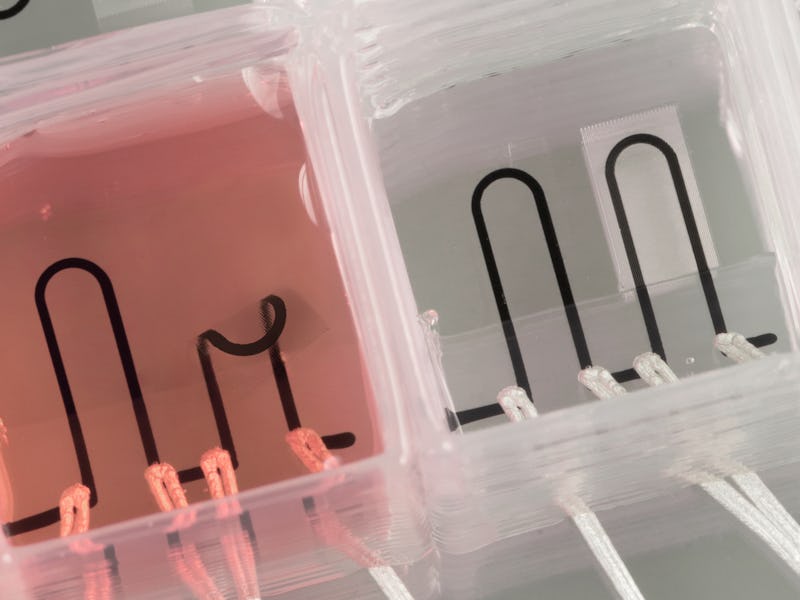
Harvard researchers announced Monday that they have created a 3D-printed “heart-on-a-chip” that promises to revolutionize medical testing. Soon, instead of conducting studies on animals, doctors might be able to use the technology to better understand what’s happening inside our bodies.
Each heart-on-a-chip is made from a variety of materials, including a series of integrated sensors that measure activity of the muscles that comprise the microchip’s artificial heart. They’re 3D-printed on a micrometer scale — a strand of spider web silk is between three and eight micrometers thick. The pathways on these devices are even smaller.
The “heart” on the microchip is made from the same tissues that make up the heart beating in your chest. These tissues behave like their natural counterparts, too: Examining them under a microscope reveals that the muscles “beat” just like their much larger counterparts. The result is an artificial heart that feels and acts like the real thing. It’s made using human tissue, and has a similar architecture.
The team explained that these chips won’t be used to create viable organs. Instead, they will be used by medical researchers, who will be able to study tissue from human organs rather than animal tissue, which might not have the same characteristics.
Harvard’s new heart-on-a-chip follows the similar lung-on-a-chip, made by the same team in 2015, and the liver-on-a-chip MIT made in January. These devices share a goal: helping us learn about ourselves.
“A key motivation [of this research] is to use human engineered tissues as test platforms for studying diseases and identifying new drugs and toxic compounds,” Harvard research associate Johan Lind told Inverse. “This will serve as a future complement or even alternative to animal testings.”
This heart-on-a-chip could be used to help understand cardiac diseases, effects of different stressors on heart tissues, and more. The heart-on-a-chip isn’t exactly like a human heart, but it’s good enough to be used in medical studies.
This heart-on-a-chip differs from other organs-on-chips in two ways — the manufacturing process, and the way it makes data available to researchers. It was made using multi-material 3D-printing, with six specialized inks, which allowed the process to be automated, while also making it easier for the team to receive information from the chip.
Harvard’s team compared this to more “expensive and laborious” production methods for other organs-on-chips. Those devices are “built in clean rooms, using a complex, multi-step lithographic process, and collecting data requires microscopy or high-speed cameras.” Being able to 3D-print these chips makes them far easier to produce than before.
As these devices become easier to create, cheaper to manufacture, and better able to share information with researchers, they could help end testing on live subjects. That will allow for new types of tests and more humane medical studies.
It could also have other benefits. The American Society of Mechanical Engineers said that “organs on chips could fundamentally alter how life scientists study human physiology, disease processes, and new drug candidates.”
“We are particularly interested in using our platform to understand pediatric heart diseases, and help develop cures for these,” Lind told Inverse. He also said that while similar production methods could work for other organs-on-chips, the team is currently focused on larger-scale manufacturing, and that while “some lessons learned might be useful for future bio-printing of organs for implants, it will be indirectly.”