A “remarkable” finding links a common vitamin to fighting brain cancer
A new study serves as a step towards better treatment for glioblastoma.
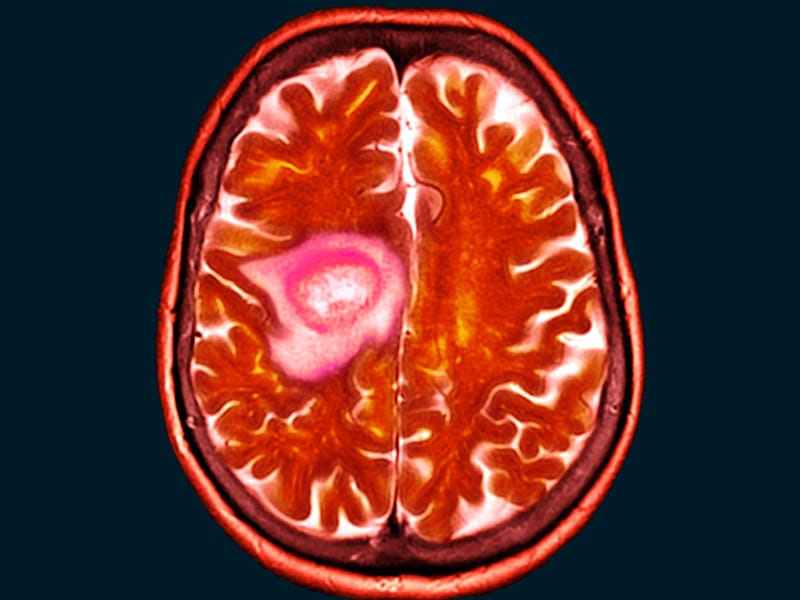
Glioblastoma is the most commonly diagnosed – and most lethal – kind of malignant brain tumor. Surgery, radiation, and chemotherapy can help slow their growth, but the tumor almost always returns. Roughly 18,000 people in the United States receive a diagnosis of glioblastoma every year; the median survival prognosis is less than fifteen months.
Efforts so far to come up with a more effective treatment have been, by and large, unsuccessful. But a new study in mice offers hope for a diagnosis that, at present, is often a death sentence.
In the study, a common vitamin called niacin, also known as vitamin B3, was seen to reprogram immune cells in the brain, in turn boosting the cell’s ability to fight off the tumor.
The research was published Wednesday in the journal Science Translational Medicine.
The finding that niacin had the ability to rejuvenate the immune system so as to suppress brain cancer was “remarkable”, says study author V. Wee Yong, a professor at the University of Calgary's Cumming School of Medicine.
The research team’s ultimate goal is to “make dents in the fight against glioblastoma,” Wee Yong tells Inverse. “It is by making several dents that we will ultimately succeed in controlling this aggressive cancer.”
Why glioblastoma is so aggressive — What makes glioblastoma so good at resisting treatment is thought to be attributable to a subpopulation of cells, called brain tumor-initiating cells, or BTICs. These cells possess “stem cell-like” properties, and are extremely adept at regrowing.
Additionally, when immune cells, such as macrophages, microglia, and monocytes, enter the tumor to try and take it down, these stem cell-like cells overthrow them – and the immune cells ultimately end up promoting tumor growth.
In a cell culture experiment, the research team found that, when treated with niacin, monocytes that had been taken from glioblastoma patients were spurred back into action – they were once again able to quash the growth of the BTICs. With the help of niacin, these immune cells regained the ability to fight off the cancer-generating potential of the brain tumor stem cells.
Treatment of mice with niacin suppressed brain tumor growth and increased the lifespan of mice.
Using mouse models that had been implanted with BTICs derived from human patients to form glioblastomas, they tested how effective niacin worked in vivo. When they treated the mice with the vitamin compound, they found that the growth of the brain tumor was brought under control, and the lifespan of the mice greatly extended. When temozolomide — chemotherapy used to treat brain tumors — was used in combination with the niacin, these effects were enhanced even more.
Wee Yong says the realization that niacin works in mice serves as a step forward towards finding a way to control cancer. He hopes that other advances will build upon the discovery, “so as to overcome the incurable glioblastoma”.
The presence of niacin-treated immune cells prevent the growth of brain tumor stem cells.
As of right now, it remains to be seen whether these findings will translate to patients, Wee Yong says. But they are planning on conducting a clinical trial in humans in the future.
“We need to figure out how to use niacin optimally in patients, and whether it works, and those are the plans going forth,” Wee Yong says.
He acknowledges that a big limitation of the study was that, so far, the treatment has only been trialed in mice.
Next up: seeing if it works in humans.
Abstract: Glioblastomas are generally incurable partly because monocytes, macrophages, and microglia in afflicted patients do not function in an antitumor capacity. Medications that reactivate these macrophages/microglia, as well as circulating monocytes that become macrophages, could thus be useful to treat glioblastoma. We have discovered that niacin (vitamin B3) is a potential stimulator of these inefficient myeloid cells. Niacin-exposed monocytes attenuated the growth of brain tumor-initiating cells (BTICs) derived from glioblastoma patients by producing anti-proliferative interferon-14. Niacin treatment of mice bearing intracranial BTICs increased macrophage/ microglia representation within the tumor, reduced tumor size, and prolonged survival. These therapeutic outcomes were negated in mice depleted of circulating monocytes or harboring interferon- receptor–deleted BTICs. Combination treatment with temozolomide enhanced niacin-promoted survival. Monocytes from glioblastoma patients had increased interferon-14 upon niacin exposure and were reactivated to reduce BTIC growth in culture. We highlight niacin, a common vitamin that can be quickly translated into clinical application, as an immune stimulator against glioblastomas