Scientists Are Making Organoids Out of Amniotic Fluid
These tiny organs could revolutionize personalized medicine for the unborn during pregnancy.
In the last decade or so, organoids have taken the scientific world by storm. From mini-brains to hearts and even boobs, these miniature, simplified versions of human body parts are expanding our understanding of the intricacies involved in how our bodies work and how we can study them better.
Stem cells are the usual ingredients scientists reach for when cooking up an organoid. But now, a group of researchers led by the University College London in the UK have found a way to use fetal cells found free-floating in amniotic fluid.
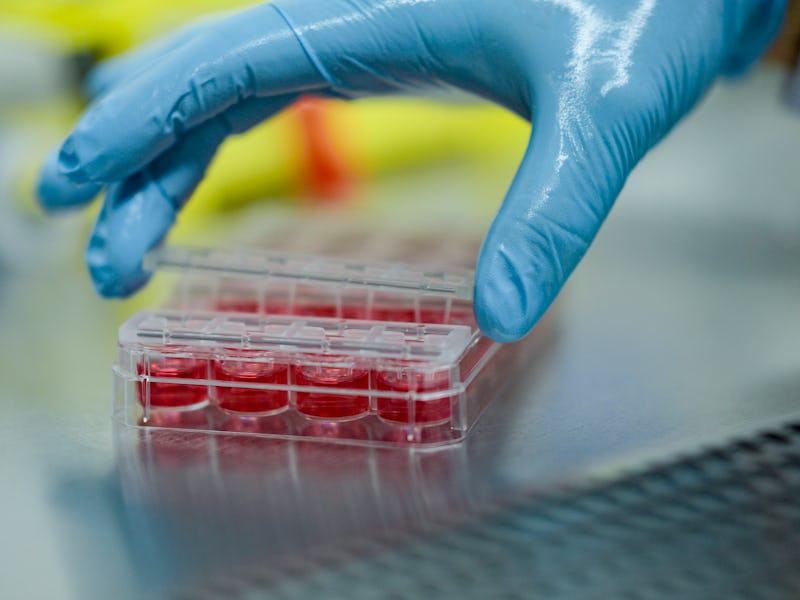
In a study published Monday in the journal Nature Medicine, some fetal epithelial (aka skin) cells shed into amniotic fluid during pregnancy carry the potential to form specific organoids. The researchers collected these cells from pregnant individuals who were at various stages of their pregnancy, put these cells into Petri dishes containing three-dimensional scaffolds, and, over several weeks, watched the cells self-assemble into organoids functionally resembling the small intestine, kidney, and lung.
In a separate experiment, the researchers also make lung organoids from epithelial cells collected from the amniotic fluid of babies with congenital diaphragmatic hernia (or CDH), a rare condition present at birth where the muscle partitioning the chest from the abdominal cavity is defective. This was done to better understand how congenital defects unfold during fetal development and may pave an avenue for treating these conditions prenatally before a child is born.
“Organoids are entering more and more the pharmaceutical industry, the clinic, and so on, but most of these are focusing on adults,” Mattia Gerli, the paper’s first author and a lecturer in stem cell science and biomaterials at the University College London, told reporters in a press briefing last week. “Here, we have for the first time the possibility of bringing the technological developments being brought forward in the pharmaceutical industry for adults… [such as] drug testing and disease modeling mechanisms, back into fetal development because, for the first time, we can actually access the fetus without touching the fetus.”
Crafting an organoid
Amniotic fluid is a clear, yellowish liquid that surrounds and cushions the fetus during pregnancy and comes from water in the mother’s body but is mostly baby pee after 20 weeks of gestation. Aside from containing nutrients, hormones, antibodies, and other components that keep the unborn baby hale and hardy, there’s quite a lot of cellular debris flecked off by the fetus, about one to two percent of which are viable, said Gerli.
Despite amniotic fluid cells being used in the last four decades for prenatal testing like amniocentesis (used to diagnose genetic disorders), a detailed catalog characterizing these cells has yet to be fully captured. For scientists, because these amniotic fluid cells present as a potentially untapped resource of still-developing fetal cells from which to make organoids, there have been talks of, but so far, no attempts to use them, Paolo De Coppi, a pediatric surgeon at the University College London and Great Ormond Street Hospital for Children, told reporters during the press briefing.
“As a pediatric surgeon interested in congenital malformations, I’ve been interested in amniotic fluid [as a source for organoids] for quite some time,” said De Coppi. “In 2007, we described in Nature Biotechnology that it was possible to derive mesenchymal cells [a type of stem cell] from amniotic fluid. These cells were already being used for prenatal diagnosis, but we and others have shown these cells can form tissues like bone, cartilage, and adipose [tissue].”
In their latest study, the researchers examined and isolated cells from amniotic fluid collected from pregnant individuals during their prenatal visits to the University College London Hospital. These individuals were each at various stages of their pregnancy, ranging anywhere from 12 to 34 weeks gestation.
Around 60 to 70 percent of the living cells they found were epithelial, or skin, in origin. Zooming in even further, Gerli, De Coppi, and their colleagues found some of these cells bore chemical markers signifying them as progenitors, immediate descendants of stem cells that, when they divide and multiply, form into specific tissues and organs.
These progenitors were then housed in special Petri dishes that allowed them to move around and grow in three dimensions. After a few weeks, the researchers ran DNA sequencing and other tests to determine what sort of organs these tiny versions were in the process of becoming.
“These [tests] showed us that we had fetal organoids derived from amniotic fluid resembling kidney, small intestine, and lung,” said Gerli.
Modeling and monitoring fetal conditions
Encouraged by these results, the researchers explored whether they could engineer lung organoids from cells collected from the amniotic and tracheal fluid of babies with congenital diaphragmatic hernia. This birth defect affects around 1,600 children born yearly in the U.S. and results in the abdominal organs pressing against the lungs, preventing them from developing properly and causing breathing difficulties for the child at birth. Mortality is significantly high, anywhere from 30 to 60 percent, and as much as 89 percent if other chromosomal or structural abnormalities are present at the same time.
“The gold standard for diagnosis at the moment is imaging – so ultrasound and MRI – and genetics. Unfortunately, we can say very little about the function, so the organs that may be [malformed],” said De Coppi. “With this study, we tried to understand a bit more about these organs… these also give us access to a gestational age where you don’t normally have access to fetal material.”
As with the other organoids, the researchers managed to create lung organoids that demonstrated the same damaging anatomical patterns seen with congenital diaphragmatic hernias. In organoids made from cells where the fetus had undergone the conventional surgical procedure to fix the birth defect, called fetoscopic endoluminal tracheal occlusion, which is a balloon used to prevent the lungs from collapsing, these organoids resembled normal organoids not made from the amniotic cells of these babies.
“[This] indicated that the fetal procedure is sort of normalizing the phenotype of these organoids,” said Gerli. “This is basically an indication that our platform could be utilized to monitor disease and model this disease.”
While this research is still in its preliminary stages, both Gerli and De Coppi are hopeful that their method of using amniotic fluid-derived epithelial cells will provide an alternative means for making organoids, especially geared toward fetal development research. For example, these organoids could help clinicians personalize which drugs work better for which patients, as not everyone responds the same way to a drug.
Gerli sees organoids made from amniotic fluid cells as a gateway to making this technology more accessible and applicable since the cost of DNA sequencing and other tests used to identify cells is going down, and manufacturing these mini-organs takes only a matter of weeks.
“Organoid derivation from amniotic fluid takes about four to six weeks. This timeline is applicable for prenatal therapies,” said Gerli, “so I think we’re really excited about the possibility of implementing personalized medicine starting from these organoids.”