Necrotizing fasciitis: How to avoid the rare and fast-spreading infection
Why flesh-eating bacteria can show up in the most unlikely of places.
Jayne Sharp walked into Knoxville, Tennessee’s Jazzy Nail Bar looking for a manicure and walked out with a deadly infection. While she was getting her nails done, Sharp’s thumb was nicked. Two hours later, her thumb started throbbing and she began experiencing flu-like symptoms.
She had the wound checked out by a nurse practitioner who ran a flu test, which came back negative. So she went home, took a nap, and when she awoke the swelling had spread from her thumb, to her entire hand, and up her arm. When the nurse practitioner called back to check in, what needed to be done was obvious: Sharp needed to go to the emergency room, and now.
The culprit, which moves quickly and kills 1 out of 4 people infected, was necrotizing fasciitis (NF).
Now, nearly nine months after the event, Sharp is missing a part of her thumb, but everything considered, she’s okay. But her story, which went viral this week, prompts the question: How can one even encounter NF at the salon?
Does necrotizing fasciitis actually eat your flesh?
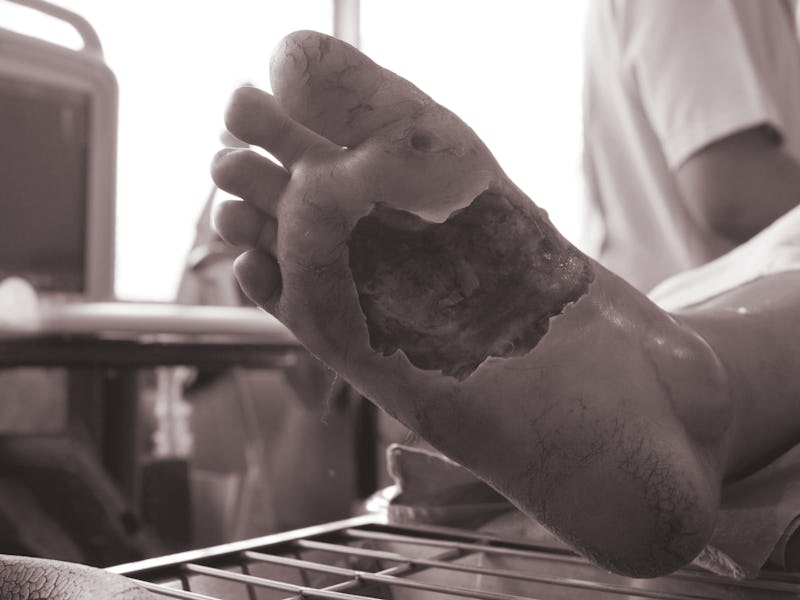
Let’s start with the basics: Necrotizing fasciitis (NF) is a rare, destructive bacterial infection. Commonly referred to as a “flesh-eating bacteria,” NF does not literally eat flesh but kills soft tissue, muscle, and skin as it rapidly spreads throughout the body.
More than one type of bacteria can cause NF, but public health experts believe group A Streptococcus is the most common cause. Most people who carry these bacteria don’t become sick, and it’s not fully understood why they can lead to NF.
A bacterium called Vibrio vulnificus can also also cause NF. It’s a natural inhabitant of coastal waters and was linked to a handful of infected patients diagnosed this summer on the East Coast. While Sharp was diagnosed with NF, it is not known which type of bacteria was linked to her illness.
A slide of biopsied necrotizing fasciitis.
NF is extremely rare and only 4 out of 1 million people will die from it. Anyone can contract NF, but elderly folks, diabetic people, small children, and those with weakened immune systems, kidney disease, cirrhosis, or cancer are more susceptible than others.
According to the CDC, most cases of necrotizing fasciitis occur randomly, and an infected person rarely passes the infection on to other people. From 2003 to 2013, there were only about 10,000 NF-related deaths reported in the United States.
Where is NF found?
It’s difficult to say because of the variety of bacteria that can drive the disease. Accordingly, the Centers for Disease Control and Prevention recommend staying away from hot tubs, swimming pools, and natural bodies of water like lakes and oceans if you have an open wound or skin infection.
“A lot of the bacteria that cause necrotizing fasciitis live on the skin and are kind of ubiquitous,” Swalpa Udit, M.D., Ph.D., a clinical infectious disease doctor at Massachusetts General Hospital and research fellow in immunology at Harvard Medical School, tells Inverse. “A lot of times, the infection is probably microbial and caused by a bunch of different organisms.”
Tiny cuts (like the sort that Sharp got at the salon), small wounds, insect bites, surgical wounds, muscle contusions, and burns can be openings for these types of bacteria to burrow into the fascia or skin, and spread like they’re speeding down a highway throughout the body.
Isaac Chiu, Ph.D., assistant professor of microbiology and immunobiology at Harvard Medical School, revealed in his research that there are clever ways certain bacteria shut down the body’s immune response fighting their destruction.
“The bacteria secrete a toxin that we identified called streptolysin, which causes pain, causes a nerve signal which blocks the immune system, and kills immune cells,” Chiu tells Inverse. “It causes a lot of damage to tissue.”
Eventually, Chiu says, the hope is that the connection between bacteria, immunity, and nerve signaling could inform new therapies for NF like antibodies to block the toxin or ways to block the nerve signal which depresses the immune system.
Surviving NF
In the first minutes and hours of infection of NF, the surface of the skin can look normal, even healthy. But beneath the surface, NF is spreading and killing healthy tissue. The pain often comes first. Patients report experiencing extraordinary levels of pain, disproportionately severe to the pain of merely a wound. Along with pain, there are other major warning signs to watch out for: Udit explains that “crescendoing pain,” the skin changing color, blisters, and skin making “crackling sounds” are all things to look out for.
Vibrio vulnificus, a flesh-eating bacteria responsible for several beach-based infections this year.
Any of these symptoms accompanied by feeling systematically sick, like the flu or a fever, should prompt you to seek medical care. Dizziness, fatigue, diarrhea, or nausea can also appear as the infection progresses, according to the CDC.
The sooner a patient seeks medical treatment, the higher their chance of survival. Treatment often includes surgical debridement or removal of dead and infected tissue, sometimes repeated, which can result in minor scarring or even partial and total amputation of limbs. NF patients receive a broad range of antibiotics, often through an IV. There is currently no vaccine to ward it off. If not treated quickly, patients can experience systematic organ failure within 12-48 hours after becoming infected.
The best line of defense against NF is good wound care: Wash wounds with soap and water, and change bandages or wound dressing frequently.
Necrotizing fasciitis is rare, but if you notice warning signs — extreme pain, swelling, or redness — after surgery or injury, go see a doctor as soon as possible. People have reason to be worried if they suspect infection. But the odds that a person will become infected in their lifetime is extremely low. So take note of the symptoms and be careful if you have an open wound, but there’s no need to walk through life fearful of contracting a “flesh-eating” disease.